
Prof. Mariano Sanz
Catedrático de Periodoncia en la Universidad Complutense de Madrid.
Periodontitis is a multifactorial chronic inflammatory disease associated with a dysbiotic oral microbiome. If left untreated, periodontitis can lead to the progressive destruction of the tooth supporting tissues untimely resulting in tooth loss. Periodontitis is a highly prevalent chronic disease, being the sixth-most prevalent condition in the world. According to recent epidemiological data, severe periodontitis is estimated to affect 11.2% of the global adult population, with country-specific prevalence estimated at 8.5% in the USA. The recently introduced classification of periodontal diseases has identified well‐defined clinical entities using clear criteria being able to link diagnosis with prevention and treatment, thus moving towards precision and individualised dentistry.
Once the diagnosis of periodontitis is made, periodontitis cases need to be characterised by the newly introduced process of staging and grading (Papapanou, Sanz et al., 2018). Periodontitis stages are a simple description of the severity and complexity of management of the individual case, while periodontitis grades capture the risk of progression and the risk factor profile. This newly introduced system aims to identify, on one side of the spectrum, cases as early as possible through the identification of initial signs of attachment loss (stage I) and on the other side the more advanced cases requiring more advanced periodontal therapy (stage III) or complex periodontal and oral rehabilitation (stage IV). Introducing this new classification in clinical practice requires careful planning and the introduction of a novel, yet simple, way of thinking, which introduces new diagnostic tools and a new decision‐making algorithm to support the process leading to diagnosis and case definition (Tonetti and Sanz 2018).
When the evaluation of Clinical Attachment Loss (CAL) is higher than 5 mm or if the BL affects the middle third of the root or beyond, the diagnosis is either stage III or IV periodontitis. Similarly, if CAL is <5 mm, the clinician should look for the presence of class II or III furcation involvement of intrabony lesions, which when present will guide to the diagnosis of Stage III and IV. When BL affects the middle third of the root or beyond and CAL is 5 mm or more, if PTL is 4 teeth or less and in the presence of 10 or more occluding pairs, in the absence of bite collapse, drifting, flaring or a severe ridge defect, then the diagnosis is stage III. When BL affects the middle third of the root or beyond and CAL is 5 mm or more, if PTL is more than 4 teeth and in the absence of 10 occluding pairs, or when existing bite collapse, drifting, flaring or a severe ridge defect, then the diagnosis is stage IV.
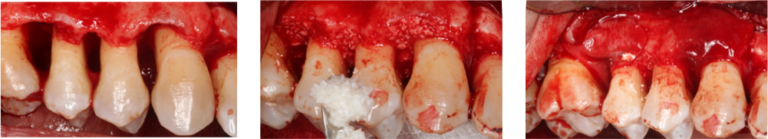
In stage III periodontitis the absence of significant tooth loss (less than 4 teeth) and functional alterations focus the treatment in advanced periodontal treatment. The presence of deep probing depths and extensive CAL > 5 mm requires the need of surgical periodontal therapy and the frequent presence of intrabony lesions and furcation lesions, also indicates the inclusion of periodontal regenerative interventions to restore these lesions and improve the individual prognosis of affected teeth.
In stage IV periodontitis the need of rehabilitating the tooth loss and the functional alterations characteristic of Stage IV periodontists, requires the introduction of multidisciplinary treatment beyond the advanced periodontal therapy. Depending on the specific needs, orthodontic, implant and prosthetic interventions will be required.
In this presentation, during Ticare Evidence, XI Implantology Congress, the specific modes of therapy for both stage III and IV periodontitis will be presented by describing the treatment of selected cases.


